Rapid antigen tests can detect the latest COVID-19 variants, but their performance may be weaker than it was with the original SARS-CoV-2 strains. There is a good chance that you will have to test more than once to get your first positive test.
The answer to the question “how well do antigen tests work?” is a moving target. It depends on many factors, including viral variant, test brand, and amount of virus on the swab.
For example, a recent study of early Omicron variants using Roche and Acon FlowFlex rapid antigen tests found that when viral levels in the samples were high, both brands detected roughly 90% of samples, across BA.1, BA.2 and BA.5. When viral levels were moderate, detection rates for Roche’s test dropped by 4% (from 91% to 87%) for BA.1, and dropped by 10% for BA.5 and 20% for BA.2. By contrast, performance of the Acon FlowFlex test was consistent across variants. See figure for more info.
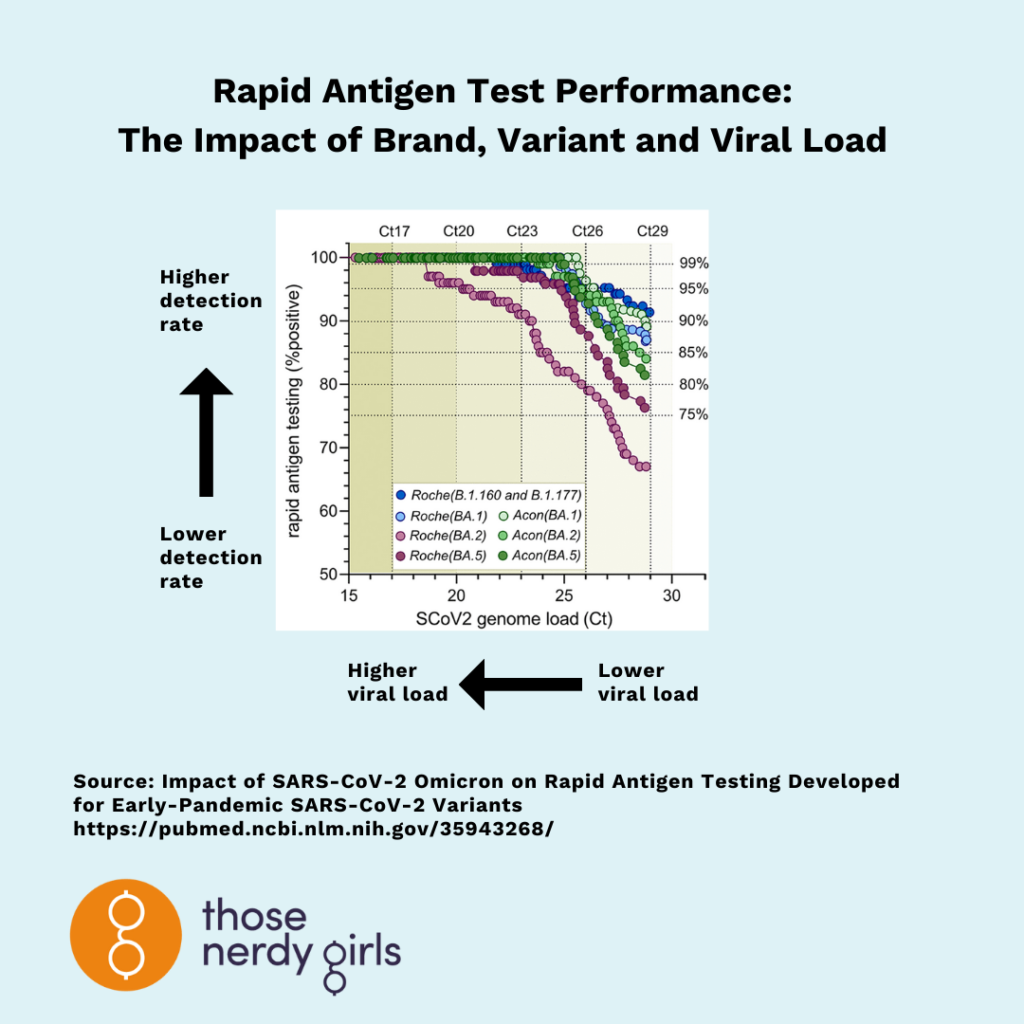
For the Kraken variant (XBB1.5), experts believe that rapid antigen test performance will be similar to other Omicron variants, though we don’t yet have any published studies. Performance will also likely vary across brands. Every brand of rapid antigen test uses a unique set of antibodies to detect a specific piece of the virus, which may or may not be mutated in each variant.
Tips for testing wisely given these limitations:
![]() Optimize timing: If you only have one test available, consider waiting 2 days from symptom onset to give the virus ample time to replicate. Viral levels often peak as symptoms wane. Be sure to and play it safe in the meantime.
Optimize timing: If you only have one test available, consider waiting 2 days from symptom onset to give the virus ample time to replicate. Viral levels often peak as symptoms wane. Be sure to and play it safe in the meantime.
A study of Delta and early Omicron variants found that a single rapid antigen test detected 60% of symptomatic cases on Day 0, and 90-95% of symptomatic cases on Days 2-4 (Day 0 = first positive PCR).
![]() Repeat if negative: If you suspect you may have COVID but test negative, re-test again in 48 hours apart. A single negative test is *not* conclusive.
Repeat if negative: If you suspect you may have COVID but test negative, re-test again in 48 hours apart. A single negative test is *not* conclusive.
A study of Delta and early Omicron variants found that antigen tests detected the virus 83% of the time with one test, and 93% of the time with two tests 48 hours apart (in symptomatic cases, Days 0-6).
![]() Consider a dual swab: The SARS-CoV-2 virus may sometimes replicate first in the throat before it takes off in the nose. A combined swab (first throat, then nose) may boost your chances of detecting COVID-19 early. Don’t feel you have to do this every time – try the nasal one first, and up your game if the virus is proving elusive.
Consider a dual swab: The SARS-CoV-2 virus may sometimes replicate first in the throat before it takes off in the nose. A combined swab (first throat, then nose) may boost your chances of detecting COVID-19 early. Don’t feel you have to do this every time – try the nasal one first, and up your game if the virus is proving elusive.
A Canadian study compared nasal swabs to combined throat/nose sampling with the Abbott PanBio test. The tests detected 68% of positive cases with nasal swabs alone but 82% of cases with dual swabs. No false positives were reported.
![]() NB: Combined swabs are NOT recommended by the FDA, but this practice is supported in the UK, Israel, and parts of Canada.
NB: Combined swabs are NOT recommended by the FDA, but this practice is supported in the UK, Israel, and parts of Canada.
![]() Hot tip: To learn about access to free rapid antigen tests in the US, check out links below for more information.
Hot tip: To learn about access to free rapid antigen tests in the US, check out links below for more information.
![]() Nerdy Bonus: Three factors that contribute to changing antigen test performance:
Nerdy Bonus: Three factors that contribute to changing antigen test performance:
![]() Changing fit. You can think of antigen tests as glass slipper (the test) and Cinderella’s foot (a viral protein called N or nucleocapsid). When the virus mutates, it’s like getting a bunion on Cinderella’s foot. It no longer fits as well. Some test brands are more affected than others, depending on their design (open toe sandals are less impacted than closed toe!)
Changing fit. You can think of antigen tests as glass slipper (the test) and Cinderella’s foot (a viral protein called N or nucleocapsid). When the virus mutates, it’s like getting a bunion on Cinderella’s foot. It no longer fits as well. Some test brands are more affected than others, depending on their design (open toe sandals are less impacted than closed toe!)
![]() Changing viral biology. An antigen test can’t detect the virus if it’s not on the swab. It may be that newer variants don’t replicate and shed in the nose until later in the infection (in some people).
Changing viral biology. An antigen test can’t detect the virus if it’s not on the swab. It may be that newer variants don’t replicate and shed in the nose until later in the infection (in some people).
![]() Changing host biology. Some experts theorize that we are getting symptoms earlier than we used to because of natural immunity and vaccines. Our immune response symptoms may show up before the virus has had a chance to replicate and make tons of copies.
Changing host biology. Some experts theorize that we are getting symptoms earlier than we used to because of natural immunity and vaccines. Our immune response symptoms may show up before the virus has had a chance to replicate and make tons of copies.
Stay safe. Stay well.
Those Nerdy Girls
————————————————————————–
US Home Testing Resources
Access to free rapid tests from US government (4 per household)
Fully covered COVID-19 rapid tests for people with US health insurance (8 pp per month)
Links:
How well to COVID-19 antigen tests work?


